Cervical cancer prevention today is based on increasingly precise and effective protocols, which guarantee accuracy, safety and comfort for the patient.
Pap smear: an exam that evolves with technology
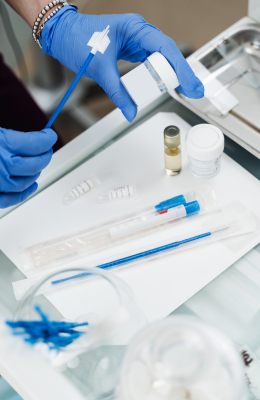
In 2026, prevention is one of the most powerful weapons to protect women’s health, detect diseases early, and significantly reduce the incidence of preventable cancers.
The Pap test is one of the main preventative screening tests. It is a cytological analysis that identifies cellular abnormalities in the cervix before they develop into cancerous lesions.
In Spain, approximately 1,900–2,300 new cases of cervical cancer are diagnosed each year, and around 600–825 deaths are attributed to this disease. Cytological screening, such as the Pap test, has been shown to help reduce both mortality and the incidence of the disease.
From a professional standpoint, it is essential to use high-quality equipment to increase diagnostic accuracy and reduce false negatives. The main instruments for performing the test correctly are:
- Gynecological speculum (disposable or reusable and sterilizable): allows visualization of the cervix. Transparent, ergonomic, and latex-free materials are preferred nowadays.
- Ayre spatula: used for collecting cells from the exocervix.
- Cytobrush or endobrush: allows collecting cells from the endocervical canal, improving the quality of the sample.
- Liquid-based cytology slides or bottles: increasingly used, liquid cytology reduces unsuitable samples and allows additional tests to be performed with the same sample.
HPV screening: accuracy and early prevention
The HPV (Human Papillomavirus) test is one of the most important screenings for women over 30. This test is more sensitive than the Pap test for identifying women at risk, allowing the problem to be detected before cellular abnormalities appear.
Approximately 8 out of 10 women come into contact with HPV at least once in their lifetime, but in most cases the infection clears up spontaneously.
The sample collection is performed similarly to the Pap test, using instruments such as:
- Combined devices for cervical sampling (spatula + brush): allow for complete sampling in a single procedure.
- Tube with preservation medium: keeps viral DNA stable until laboratory analysis.
- Molecular analysis systems: highly sensitive automated platforms capable of identifying and genotyping the main types of oncogenic HPV.
In 2026, many laboratories use integrated systems that allow, in the case of HPV positivity, the triage Pap test to be performed directly on the same sample.
HPV self-sampling: an increasingly widespread innovation

One of the most relevant innovations in recent years is the introduction of self-sampling for HPV testing, designed to increase participation in screening, especially among women who attend gynecological check-ups less frequently.
Instruments for self-sampling:
- Vaginal swabs or dedicated devices certified as medical devices;
- Disposable kits with clear instructions for home use;
- Transport containers compatible with molecular analysis systems.
Numerous studies confirm that, if used correctly, self-sampling offers results comparable to clinical sampling for HPV detection.
Colposcopy and follow-up: in-depth tools
In the event of abnormal results, the screening process includes secondary tests, which are essential to confirm or rule out the presence of precancerous lesions. Approximately 5-10% of women screened are referred for further testing.
Instruments used in monitoring:
- Colposcope: a high-resolution optical instrument that allows magnified observation of the cervix, with variable magnifications of up to 10–20 times, allowing the identification of even minimal alterations of the epithelium.
- Reactive solutions (acetic acid and Lugol’s solution) to highlight suspicious areas.
- Biopsy forceps: These allow for targeted tissue sampling in altered areas, essential for histological confirmation. Only a small percentage of biopsies are subsequently associated with high-grade lesions, thus avoiding unnecessary treatments.
- Electrosurgical or laser devices, used in the treatment of precancerous lesions.
For health centers, doctor’s offices and gynecological clinics, investing in reliable, certified and technologically advanced devices means improving diagnostic quality, reducing unnecessary interventions and contributing concretely and effectively to cancer prevention.

I am an MBBS student and medical content writer specializing in health education, medical research, public health awareness, and informational guides. With a strong foundation in clinical knowledge and evidence-based medicine, I write accurate, SEO-optimized, and reader-focused articles. My content covers healthcare topics, medical updates, government welfare programs, and educational resources to help readers access reliable and up-to-date information. I am committed to delivering trustworthy, well-structured, and search-engine-friendly content that adds real value.